Calculation of the LDL-cholesterol to HDL-cholesterol ratio provides a better assessment of cardiovascular risk than measuring either biomarker alone.
Increased ratio reflects
In general,
These levels and ratios can provide general guidelines. However, cardiovascular risk can be further defined using additional information such as free radical load, oxidized LDL, inflammatory markers, macrophages, and foam cells.[ii]
Hao et al 2014[iii]: Atherosclerosis schematics: the presence of ox-LDL in the intima causes monocytes to migrate from the lumen into the intima. Monocytes differentiate into macrophages which endocytose ox-LDL and become foam cells. SMCs are attracted from the media into intima by chemotaxis and haptotaxis. Cytokines released by macrophages, foam cells and SMCs activate T cells. T cells enhance activation of macrophages. HDL helps prevent atherosclerosis.
A retrospective study following 1,784 individuals undergoing coronary angiography (CAG) divided subjects into those with a LDL:HDL cholesterol ratio of less than 2.33 (mean of 1.79) and those with a ratio of 2.33 or greater (mean of 3.11).
A 23-year prospective cohort study of 2,626 middle-aged men found that an elevated LDL:HDL ratio was independently associated with increased risk of sudden cardiac death (SCD), a phenomenon that accounts for half of all cardiovascular deaths.
Cardiometabolic health should always be assessed as a whole and evaluation of glucose tolerance is prudent when assessing cardiovascular risk. In one cross-sectional study of 2,680 participants, the mean LDL:HDL cholesterol ratio of individuals with normal glucose tolerance was 2.13 while the ratio was 2.56 for those with impaired glucose regulation and 2.6 for those diagnosed with type 2 diabetes.[vi]
There may be some risk with a lower LDL:HDL in some disorders as a lower ratio (1.52 or less) was observed in those suffering hemorrhagic transformation (HT) following an acute ischemic stroke than in those who did not experience HT.[vii]
| Clinical Implications High | Clinical Implications Low |
|
Cardiovascular disease risk increase Familial hypercholesterolemia [viii] Sudden cardiac death |
Reduced risk of cardiovascular disease Reduced risk of sudden cardiac death Hemorrhagic transformation |
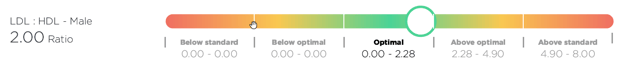
Good news! The LDL:HDL ratio is now being automatically calculated by the Optimal DX software if both the LDL and HDL are added into the system. No need to do any conversions as the software will do this for you and will now show the result in the Blood Test Results Report:
However, if you simply want to do the calculation manually then please follow these instructions:
The LDL:HDL ratio is calculated by dividing the LDL result by the HDL result.
Here's an example:
LDL is 105 and the HDL is 52: 105/ 52 = 2.02
So, the LDL:HDL Ratio in this example is 2.02
[i] Millán, Jesús et al. “Lipoprotein ratios: Physiological significance and clinical usefulness in cardiovascular prevention.” Vascular health and risk management vol. 5 (2009): 757-65. [R]
[ii] Hao, Wenrui, and Avner Friedman. “The LDL-HDL profile determines the risk of atherosclerosis: a mathematical model.” PloS one vol. 9,3 e90497. 12 Mar. 2014, doi:10.1371/journal.pone.0090497 [R]
[iii] Hao, Wenrui, and Avner Friedman. “The LDL-HDL profile determines the risk of atherosclerosis: a mathematical model.” PloS one vol. 9,3 e90497. 12 Mar. 2014, doi:10.1371/journal.pone.0090497 [R]
[iv] Zhao, Y., et al. "The LDL-C/HDL-C ratio and 4-year risk of coronary artery disease: a retrospective study." (2020). [R]
[v] Kunutsor, Setor K et al. “Is High Serum LDL/HDL Cholesterol Ratio an Emerging Risk Factor for Sudden Cardiac Death? Findings from the KIHD Study.” Journal of atherosclerosis and thrombosis vol. 24,6 (2017): 600-608. doi:10.5551/jat.37184 [R]
[vi] Guo, Wen et al. “Diagnostic values and appropriate cutoff points of lipid ratios in patients with abnormal glucose tolerance status: a cross-sectional study.” Lipids in health and disease vol. 18,1 130. 1 Jun. 2019, doi:10.1186/s12944-019-1070-z [R]
[vii] Wang, Yanan et al. “Reduction in the Ratio of Low-density Lipoprotein Cholesterol to Highdensity Lipoprotein Cholesterol is Associated with Increased Risks of Hemorrhagic Transformation in Patients with Acute Ischemic Stroke.” Current neurovascular research vol. 16,3 (2019): 266-272. doi:10.2174/1567202616666190619151914 [R}
[viii] Panagiotakos, Demosthenes B et al. “Importance of LDL/HDL cholesterol ratio as a predictor for coronary heart disease events in patients with heterozygous familial hypercholesterolaemia: a 15-year follow-up (1987-2002).” Current medical research and opinion vol. 19,2 (2003): 89-94. [R]